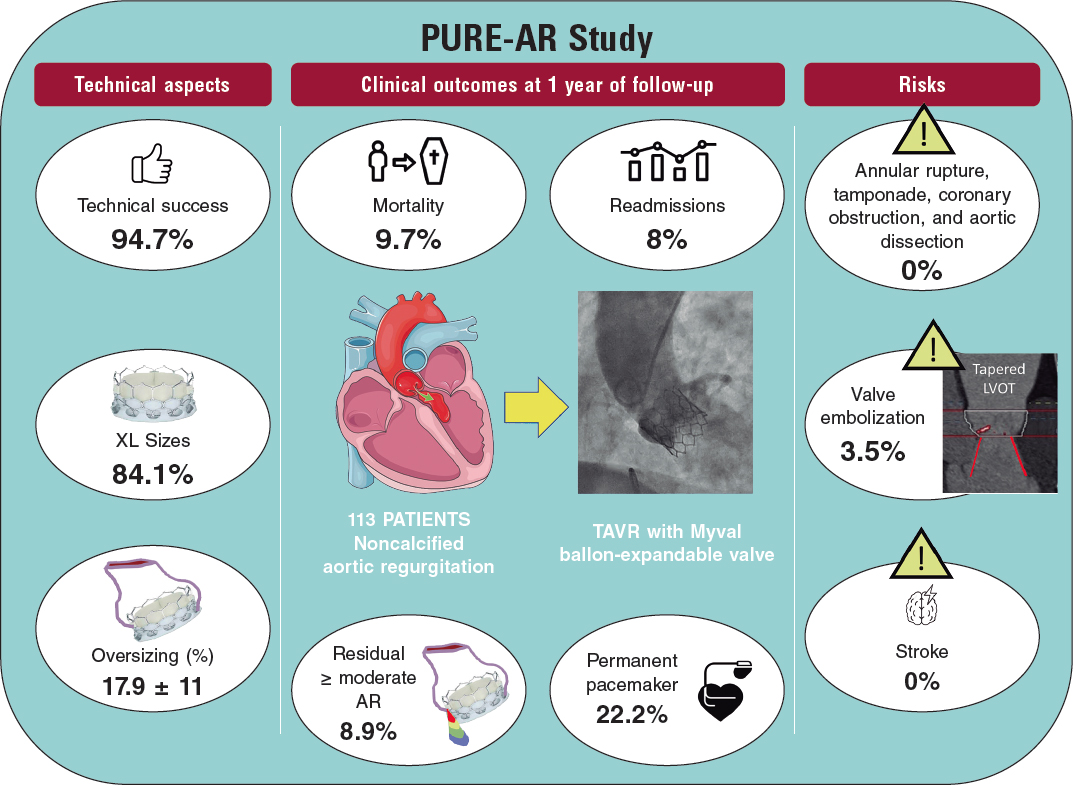
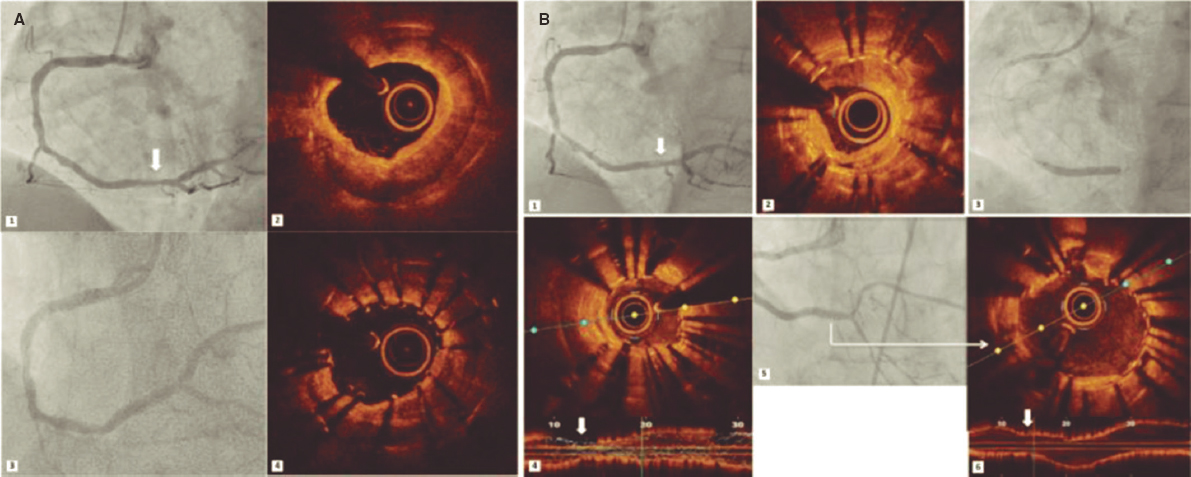
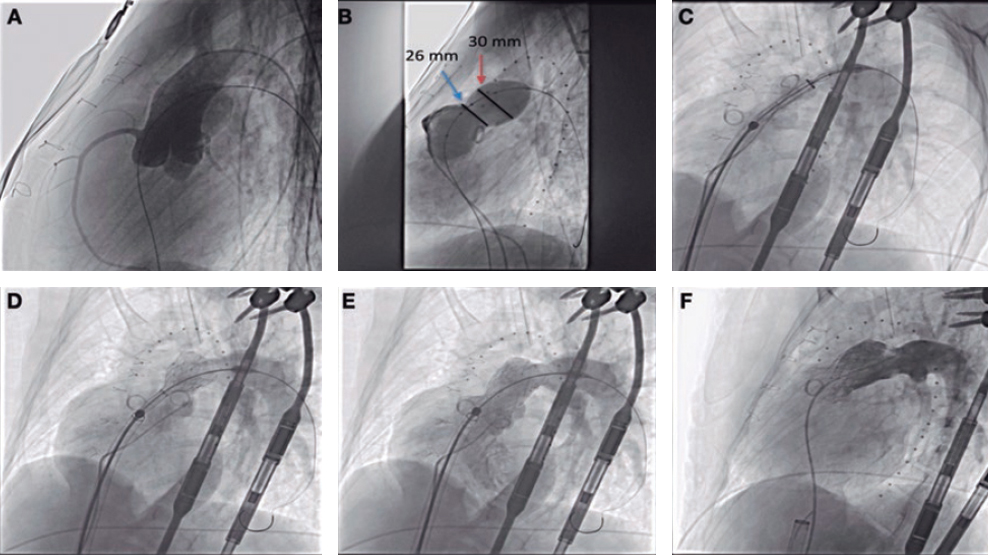
A 41-year-old woman presented with an inferolateral ST-segment elevation myocardial infarction. Coronary angiography confirmed the presence of a long narrowing involving the right coronary artery posterolateral branch (figure 1A, white arrows). Spontaneous coronary artery dissection was suspected and optical coherence tomography (OCT) imaging was considered by the operator for confirmation purposes. Advancing the OCT catheter was difficult due to lack of support and it was decided to only interrogate the proximal aspect of the branch (figure 1B, arrow). OCT revealed the presence of an intramural hematoma without entry tear (figure 1C; asterisks denote wire artefact). At that moment the patient complained of chest pain that remained after removing the OCT catheter. The presence of functional branch occlusion (figure 1D, asterisk), with Thrombolysis in Myocardial Infarction (TIMI) grade 1 flow, was confirmed. Coronary flow was re-established through gentle dilation (4 atm) using a 1.5 mm balloon. Final TIMI grade 2 flow was achieved (figure 1E, asterisks) and the patient became asymptomatic. Her subsequent clinical course was uneventful. Coronary angiography performed 3 months later confirmed the complete healing of the dissected segment (figure 1F, arrows).
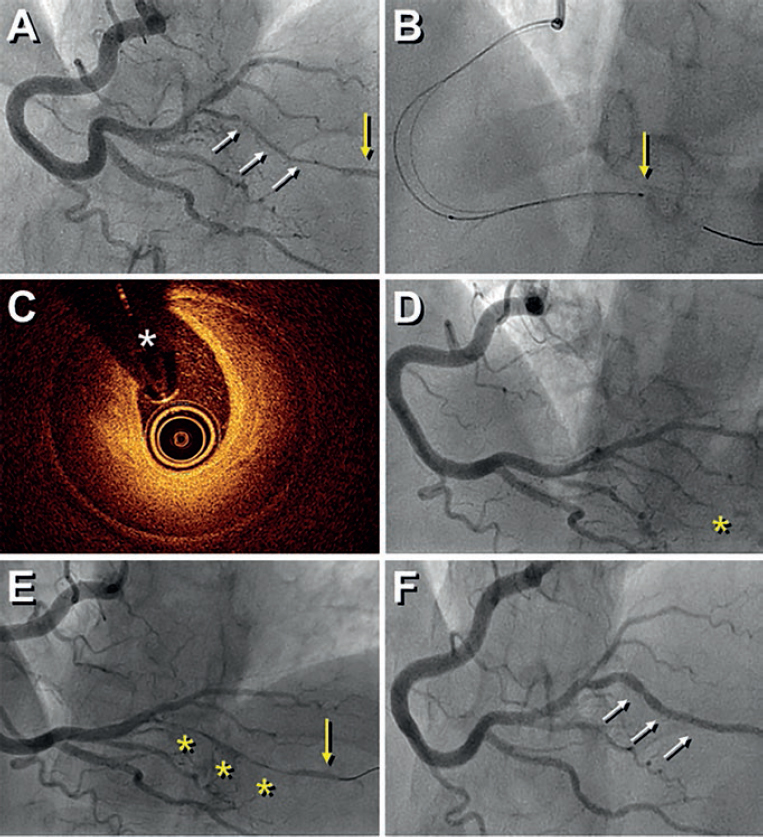
Figure 1.
Diagnosing spontaneous coronary artery dissection can be challenging in the absence of the classical dual-lumen pattern. OCT imaging is considered safe and, therefore, recommended for selected patients to confirm the diagnosis. Our findings illustrate that extra care is required while acquiring images in these frail and disrupted vessels. OCT should only be considered when the diagnosis remains unclear, and the acquisition of images in very distal and small vessels should be avoided.
CONFLICTS OF INTEREST
F. Alfonso is an associate editor of
Corresponding author: Departamento de Cardiología, Hospital Universitario de La Princesa, Diego de León 62, 28006 Madrid 28006, Spain.
E-mail address: falf@hotmail.com (F. Alfonso).